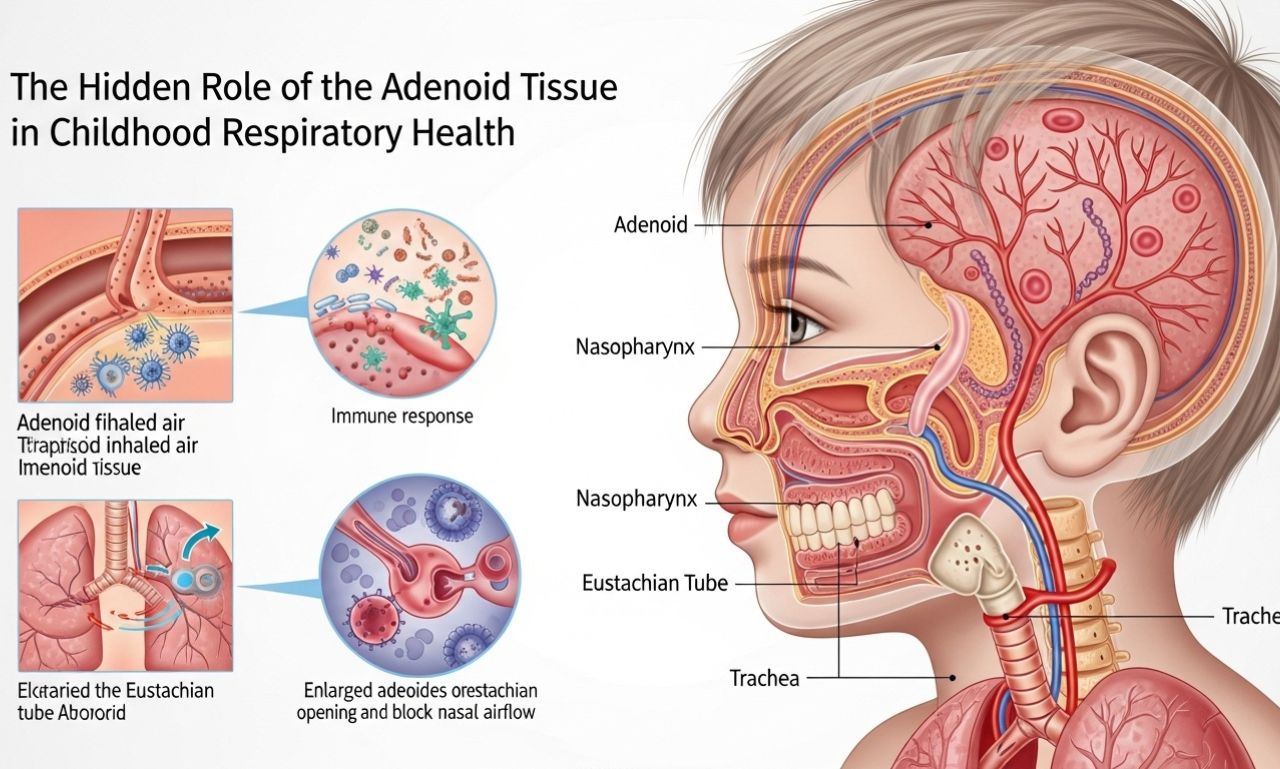
Nestled high in the throat behind the nose lies a small, often overlooked cluster of tissue that plays a giant role in a child’s developing immune system. This structure, known as the adenoidid pad, is part of the body’s first line of defense against inhaled pathogens. While most parents are familiar with tonsils, the adenoidid counterpart remains mysterious until it becomes problematic. Understanding this tissue’s function, its potential to swell, and the signs of its enlargement is crucial for maintaining proper ear function, sleep quality, and facial development in young children. Unlike tonsils, which are visible at the back of the mouth, the adenoidid location makes it a hidden player—one that can silently influence breathing, hearing, and even behavior when things go wrong.
What Exactly is the Adenoidid Structure?
The adenoidid mass is composed of lymphoid tissue, similar to lymph nodes, and forms part of Waldeyer’s tonsillar ring. From infancy through early childhood, this tissue is naturally large and active, producing antibodies to trap bacteria and viruses entering through the nasal passages. By age five to seven, the typical adenoidid volume begins to shrink, often becoming nearly invisible by adolescence. However, during its active years, recurrent infections can trigger chronic enlargement. An overgrown adenoidid pad blocks the narrow channel between the nose and throat, creating a cascade of mechanical and infectious problems. Histologically, the tissue features deep crypts lined with specialized epithelial cells that sample antigens, initiating an immune response. When healthy, this process is protective; when inflamed, the adenoidid center becomes a reservoir for biofilm-forming bacteria.
Recognizing Adenoidid Hypertrophy: Signs and Symptoms
When the adenoidid tissue expands abnormally, the symptoms are distinctly different from those of tonsillitis. The most classic indicator is persistent nasal obstruction without significant runny nose. Children with adenoidid hypertrophy breathe through their mouths constantly, snore loudly, and may experience sleep apnea—pauses in breathing followed by gasping. Another hallmark is “adenoid facies,” a long, open-mouthed facial expression with a pinched nose. Because the adenoidid pad sits near the Eustachian tube openings, swelling can block middle ear drainage, leading to recurrent otitis media and glue ear. Parents often notice muffled hearing, speech delays, or the need to repeat instructions loudly. Additionally, chronic adenoidid infection produces persistently foul breath and a nasal-sounding voice due to inadequate nasopharyngeal resonance.
How Do Doctors Diagnose Adenoidid Disorders?
Diagnosis begins with a thorough history of sleep disturbances, mouth breathing, and ear infections. However, the hidden adenoidid location prevents direct visual inspection through the mouth. Instead, an otolaryngologist uses flexible nasopharyngoscopy—a thin camera passed through the nostril—to directly visualize the adenoidid mass, assess its size relative to the airway, and note any mucus or crusting. This office procedure, while momentarily uncomfortable, provides definitive evidence. Alternatively, a lateral neck X-ray can estimate adenoidid size by measuring the soft tissue shadow against the air column. For young or uncooperative children, this radiograph is a practical first step. The doctor grades hypertrophy on a scale from 0% to 100% obstruction; anything over 75% usually warrants intervention. Additional audiometry tests rule out conductive hearing loss linked to adenoidid-related Eustachian tube dysfunction.
Non-Surgical Management of Adenoidid Enlargement
Not every enlarged adenoidid requires surgery. For mild to moderate cases, medical management focuses on reducing inflammation and treating underlying allergies or infections. Intranasal corticosteroid sprays, such as fluticasone or mometasone, directly shrink adenoidid lymphoid tissue over four to six weeks. Studies show consistent use reduces nighttime breathing difficulties and improves Eustachian tube function. Concurrently, treating environmental allergies with antihistamines or leukotriene inhibitors (like montelukast) removes chronic immune stimulation. For acute bacterial infections superimposed on adenoidid hypertrophy, a course of amoxicillin-clavulanate targets common pathogens like Streptococcus pneumoniae and Haemophilus influenzae. Importantly, if the adenoidid tissue fails to respond after three months of optimal medical therapy, or if complications like obstructive sleep apnea or hearing loss persist, surgical referral becomes necessary.
Surgical Options: The Adenoidid Removal Procedure
When conservative measures fail, an adenoididectomy—surgical removal—is the gold standard. Performed under general anesthesia, the surgeon accesses the adenoidid pad through the mouth using a specialized mirror or endoscopic guidance. Modern techniques employ microdebriders or coblator devices that remove tissue with minimal bleeding and precise margins. The procedure takes less than 30 minutes, and children typically go home the same day. Simultaneous tonsillectomy may be added if both lymphoid tissues are obstructive. Postoperative recovery involves mild throat pain, nasal congestion from swelling, and temporary bad breath due to healing eschar. Within two weeks, parents notice dramatic improvements: the child sleeps with a closed mouth, snoring ceases, and hearing often returns to normal as middle ear fluid drains. Adenoidid regrowth is rare but possible in children under three or when small remnants remain.
Long-Term Outlook After Adenoidid Intervention
The benefits of addressing adenoidid pathology extend beyond immediate symptom relief. Children who undergo successful treatment often experience accelerated catch-up growth due to normalized sleep architecture and reduced work of breathing. Speech articulation improves as the nasal airway reopens, resolving the hyponasal quality. Furthermore, preventing chronic middle ear effusion protects against potential developmental delays in language acquisition. While some parents worry about removing immune tissue, the body compensates through other lymphoid sites—lymph nodes, tonsils, and gut-associated tissue. In fact, the adenoidid role wanes naturally after age eight, making removal after this age unlikely to cause immune deficiency. The key is timely diagnosis: leaving a massively enlarged adenoidid untreated risks permanent facial skeletal changes, including a high-arched palate and dental malocclusion.
When to Seek Professional Evaluation for Your Child
You should consult a pediatric otolaryngologist if your child exhibits three or more nights per week of loud snoring, documented breathing pauses during sleep, or more than four ear infections in a single year. Additional red flags include daytime sleepiness despite adequate time in bed, poor school performance linked to inattention, or a teacher reporting that the child seems to “hear selectively.” Do not dismiss these as minor quirks; the aden-oidid tissue could be the hidden culprit. An evaluation is also warranted if your child has persistent nasal speech after age five or fails a school hearing screening. Early intervention preserves not only health but also quality of life—allowing your child to wake refreshed, breathe freely, and engage fully with the world.
Conclusion
The adenoidid tissue may be small, but its impact on growing children is immense. From immune surveillance to airway maintenance and middle ear ventilation, this lymphoid pad orchestrates critical functions during formative years. When it enlarges pathologically, it becomes a silent thief—stealing restful sleep, clear hearing, and effortless breathing. Fortunately, modern medicine offers a clear pathway: from nasal sprays and antibiotics to minimally invasive surgery, the options are effective and safe. By recognizing the signs of adenoidid distress early, parents and physicians can work together to restore normal anatomy and function. Ultimately, a healthy adenoidid is a silent guardian; a problematic one, a loud whisper. Listening carefully ensures that every child gets the breath of life they deserve.